The U.S. Food and Drug Administration (FDA) on Friday approved a pair of gene therapies for sickle cell disease, including the first treatment based on the breakthrough CRISPR gene editing technology.
The agency approved Lyfgenia from bluebird bio BLUE.O, and a separate treatment called Casgevy by partners Vertex Pharmaceuticals VRTX.O and CRISPR Therapeutics CRSP.BN.
Both the therapies were approved for people aged 12 years and older.
The Vertex/CRISPR gene therapy uses the breakthrough gene editing technology that won its inventors the Nobel Prize in 2020.
Sickle cell disease is a painful, inherited blood disorder that can be debilitating and lead to premature death. It affects an estimated 100,000 people in the United States, most of whom are Black.
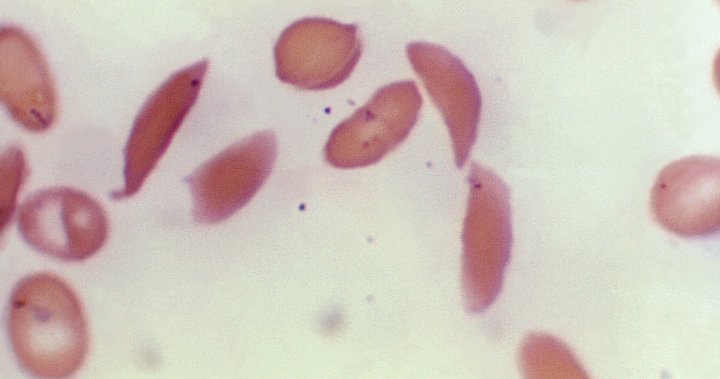
In sickle cell disease, the body makes flawed, sickle-shaped hemoglobin, impairing the ability of red blood cells to properly carry oxygen to the body’s tissues.
The sickle cells tend to stick together and can block small blood vessels, causing intense pain. It also can lead to strokes and organ failure.

U.S.-listed shares of CRISPR therapeutics were up 1.6 per cent, while Vertex Pharmaceuticals stock was down 1.4 per cent. Shares of bluebird bio were halted for trading ahead of the news.
Makers of both therapies have pitched them as one-time treatments, but data on how long their effect lasts is limited. The only longer-term treatment for sickle cell disease is a bone marrow transplant.
“I actually am very reticent to call them a cure. I prefer to call them a transformative therapy because patients will still have sickle cell disease on the other side of gene therapy,” said Dr Sharl Azar, medical director of the Comprehensive Sickle Cell Disease Treatment Center at Massachusetts General Hospital.
Bluebird bio’s sickle cell therapy is designed to work by inserting modified genes into the body through disabled viruses to help the patient’s red blood cells produce normal hemoglobin.
For Vertex’s therapy, patients must have stem cells harvested from their bone marrow. The cells are then sent to manufacturing facilities where they are edited using CRISPR/Cas9 technology. Once the cells are incubated, they are infused back into the patient during a month-long hospital stay.

Both gene therapies can take several months and involve high-dose chemotherapy, but this has potential risks of infertility.
“Not everybody who undergoes chemotherapy will end up having infertility, but the majority of them will,” said Dr Azar.
While the risk can be managed by fertility preservation methods like freezing eggs and sperm banking, this is only covered by insurance for cancer patients who undergo chemotherapy and not those receiving gene therapy, said Dr. Azar.
He said the out-of-pocket expense on it can be as high as $40,000.
FDA staff in documents released ahead of an October meeting of a panel of independent experts on Vertex’s therapy had also flagged concerns of unintended genomic alterations from the treatment.
The company plans to assess potential long-term safety risks through a 15-year follow-up study after approval.
Vertex’s CRISPR therapy is also under an FDA review for another blood disease, transfusion-dependent beta thalassemia, with a decision expected by March 30.